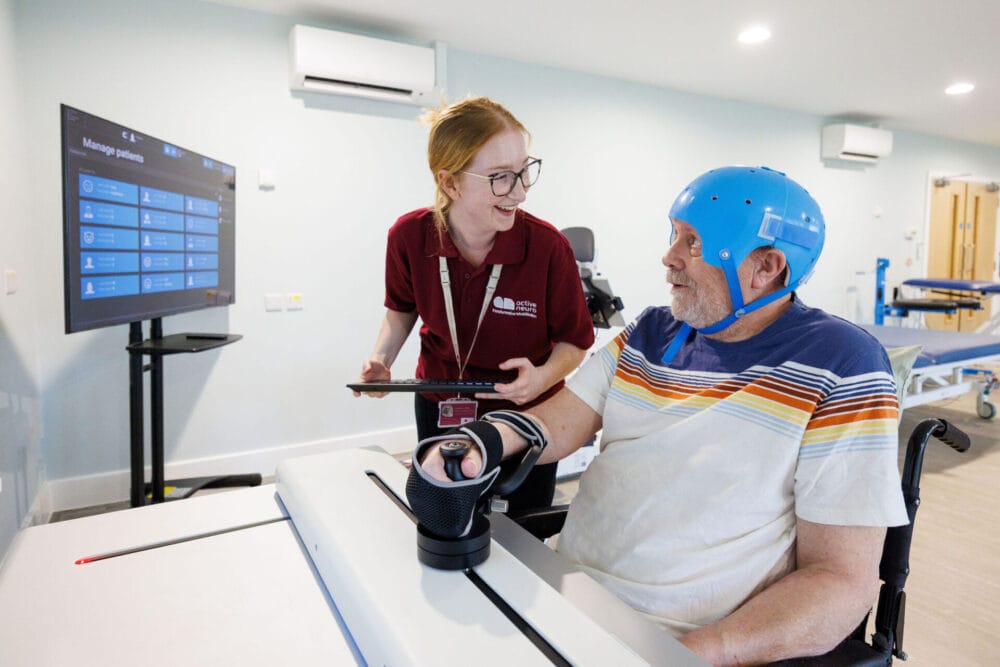
Strokes can change life instantly – affecting mobility, balance, speech, swallowing, cognition, mood and confidence. Rehabilitation supports recovery by helping people rebuild function, regain independence and adapt to new challenges with the right therapy, structure and support.
If you’re searching for stroke rehabilitation, you’re likely looking for practical answers:
- What does stroke rehabilitation include?
- How long does it take?
- Which therapies matter most?
- When is specialist neurological rehabilitation the right route?
This guide explains what stroke rehabilitation typically involves and what “good” looks like, so you can make informed decisions about pathways and next steps.
What is stroke rehabilitation?
Stroke rehabilitation is a structured programme designed to support recovery after stroke and improve day-to-day ability and independence. It can address physical, cognitive, communication and emotional needs through a coordinated plan.
Stroke rehabilitation can include:
- Physiotherapy to rebuild strength, mobility, balance, transfers and walking practice
- Occupational Therapy (OT) to support daily living skills (washing, dressing, meal preparation), fatigue management and home safety planning
- Speech and Language Therapy to support communication and swallowing needs
- Psychological support to help with adjustment, mood changes, anxiety and cognitive impact
- Nursing and care support to enable safe rehabilitation delivery and reduce risk
Specialist neurological rehabilitation services provide structured rehabilitation programmes delivered by an interdisciplinary team and focused on measurable outcomes.
Why the right rehabilitation setting matters after stroke
Stroke recovery is highly individual. Two people can have the same diagnosis and very different rehabilitation needs.
Choosing the right setting depends on factors such as:
- current mobility and functional ability
- cognition, judgement and safety awareness
- communication needs
- swallowing and nutrition risk (where relevant)
- fatigue and tolerance for therapy
- the level of therapy input required
- whether the person is safe to return home with community support
For some people, community therapy is appropriate. For others, a specialist rehabilitation placement provides the structure and multi-disciplinary input needed to progress safely.
When is specialist neuro rehabilitation appropriate after stroke?
Specialist neurological rehabilitation is often needed when presentation is more complex, for example:
- severe mobility or transfer needs requiring skilled rehabilitation handling
- cognitive impairment affecting safety, learning, or carryover of therapy strategies
- significant communication or swallowing needs
- fatigue and low tolerance requiring pacing and structured progression
- emotional or behavioural complexity affecting engagement
- longer-term or slow-stream rehabilitation needs where recovery is gradual
Specialist services may also support structured inpatient rehabilitation as part of a wider neurological rehabilitation offer.
What does a good stroke rehabilitation programme look like?
A strong stroke rehabilitation programme should be structured, goal-led and measurable.
Goal-led and focused on real-life function
Goals should be meaningful and practical, such as:
- safer transfers and mobility
- improved balance and confidence
- greater independence in personal care
- improved communication and participation
- safer swallowing and nutrition management
- improved routine tolerance and fatigue management
- preparation for discharge home or the next step in care
Multi-disciplinary by design
Stroke recovery typically requires a combination of therapies working together. Active Neuro outlines MDT-led access to Occupational Therapy, Physical Therapy, Speech and Language Therapy, Psychological Therapy, and additional therapy approaches including Neurologic Music Therapy® and Hydrotherapy.
Clear review cycles and communication
Progress should be reviewed regularly and communicated clearly to referrers and families, including:
- what is improving
- what barriers remain
- risks and how they are being managed
- what the next-step plan is
What to include in a stroke rehab referral
A good referral helps assessment happen quickly and reduces delays. Helpful information includes:
- stroke type and key history (including dates and acute pathway)
- current function (mobility, transfers, self-care)
- cognitive and communication summary
- swallowing/nutrition considerations (if relevant)
- risk summary (falls, behaviour, safeguarding)
- current therapy input and progress to date
- desired outcomes and expected timeframe
Common questions about stroke rehabilitation
How long does stroke rehabilitation take?
There is no single timeframe. Some people progress quickly; others need longer-term support. What matters is that the programme is structured, measurable, and matched to the person’s needs.
Is inpatient stroke rehabilitation available?
Some services provide inpatient rehabilitation within specialist neuro rehabilitation programmes.
Which therapies are typically involved?
Stroke rehabilitation often includes physiotherapy, occupational therapy, speech and language therapy and psychological support where needed, delivered through a coordinated MDT approach.
Next step: discuss stroke rehabilitation pathways
If you’re exploring stroke rehabilitation and want to understand the right pathway and setting, the next step is to share current needs, risks and rehabilitation goals so suitability can be assessed quickly.